by MATTHEW HOLT
I have embarked on a quest to understand why Labcorp charged me $34.95 for certain lab tests that I believed should be fully covered under the Affordable Care Act’s preventive care provisions. My insurance provider, Blue Shield of California, issued an Clarification of Benefits (EOB) stating that my co-pay was $0.
This scenario highlights the widespread confusion within the American healthcare landscape. For those interested in my earlier explorations on this topic, you can find more details in these segments: Part 1, Part 2, Part 3, adn Part 4.
You may recall that I previously paid a $50 co-pay for lab tests related to my annual wellness examination in 2024 without much concern.Though,when I received a bill for $34.94 from labcorp this year and learned from Blue Shield that my copay was supposed to be $0,it prompted me to investigate further.
I received notable help from Rhea, a senior customer service representative at Labcorp who seems as invested in resolving this issue as I am.She clarified that Labcorp aims to collect either the lower amount between $50 or the total cost of services provided. in this instance, for five tests performed on my behalf, Labcorp’s negotiated rate with Brown and Toland Physicians (an IPA affiliated with Blue Shield) came out to be $34.94—thus explaining that specific charge.
Persistent Questions arise
- Why did another lab test later show a copay of $0 according to Blue Shield’s EOB?
- If these lab tests qualify as preventive under ACA regulations, why was there any charge at all?
An In-depth Look into Coverage Issues
Rhea speculated about the first question; she suggested that Labcorp receives fixed payments per test from either Blue Shield or Brown and Toland which might have influenced how subsequent testing costs were handled compared to initial ones—but if that’s accurate, what accounts for the inconsistency with my first test?
My exploration into coverage classifications under ACA guidelines led me down an intricate path of inquiry. Rhea retrieved documentation detailing orders sent from One Medical to Labcorp which included CPT codes identifying each specific test along with corresponding diagnosis codes.
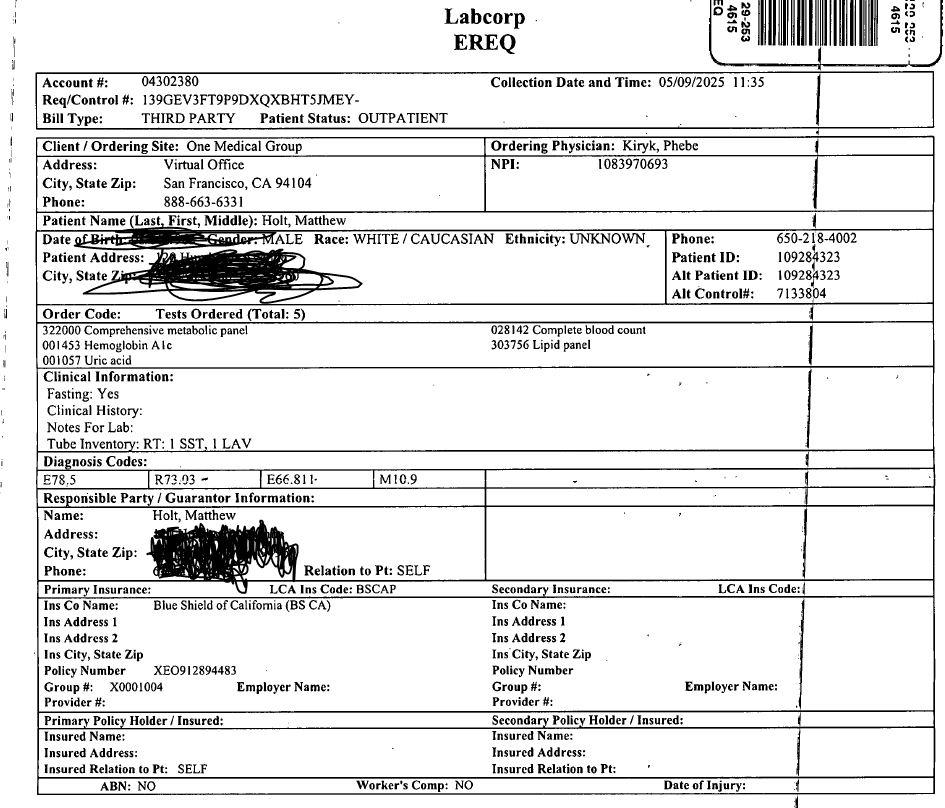
I consulted ChatGPT regarding those diagnosis codes and discovered they corresponded to:E78.5 = Hyperlipidemia (high cholesterol)R73.03 = Prediabetes E66.811 = Class 1 Obesity M10.9 = Gout.
A typical American over sixty like myself fits all these categories quite well! the CPT codes associated with my tests included complete blood count (CBC),metabolic panel analysis,hemoglobin A1C assessment,lipid profile evaluation along with uric acid measurement—directly linked back towards gout concerns.
The majority of these assessments could arguably fall within preventive care parameters; after all, CMS outlines on their website (insert link) how screenings such as blood pressure checks or cholesterol evaluations during annual wellness visits should incur no charges whatsoever!
The Ongoing Confusion Surrounding Preventive Care Designation
So why am I facing charges? According to Rhea’s insights at LabCorp ,it appears there may have been an initial error where BlueShield issued me an EOB reflecting zero copayment but failed later reprocessing once they received billing information leading up towards requesting payment instead totaling around thirty-nine dollars! Furthermore she pointed out extensive documentation outlining what constitutes preventative care according specifically outlined by California’s own version through their health plan policies available online here (insert link).
After reviewing it together via chatgpt we found E78.5 listed among applicable ICD -10 diagnostic criteria qualifying under Annual Health Appraisal Visits—a service entitled free coverage thus implying high cholesterol screenings ought not cost anything out-of-pocket!
Though upon examining page twenty-eight closely discussing pre-diabetes education programs—it does not explicitly state whether A1C testing falls within free annual wellness visit provisions nor does it clarify if recent changes made last year removed several diabetes-related coding including R73 .03 altogether noted down below page one hundred sixteen.

I won’t pretend understanding every nuance contained within such documents nor whether insurers like blue shield possess authority altering CMS directives—but something feels off about how things are unfolding here!
Moreover due lack transparency surrounding actual costs assigned per individual laboratory examination makes discerning contracted rates impractical leaving uncertainty surrounding potential discrepancies between expected versus actual expenses incurred throughout entire process.Lastly tonight brought unexpected excitement when receiving notification message indicating attachment possibly addressing grievance filed earlier through executive offices mentioned previously yet unfortunately formatting issues rendered contents unreadable—leaving me still puzzled over its implications!
Such is par for course amidst this convoluted adventure!
But fingers crossed we’re nearing clarity regarding who owes whom—and ultimately why!
Yoru guide through healthcare complexities is Matthew Holt—the founder & publisher behind THCB!